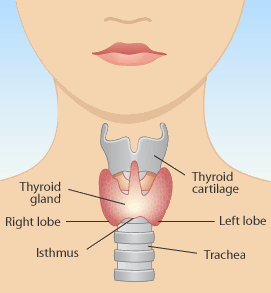
Endometriosis patients with thyroid dysfunction may have increased risk of more intense chronic pain and increased disease severity, a study suggests.
The study, “Role of thyroid dysimmunity and thyroid hormones in endometriosis” was published in the journal PNAS.
The underlying disease mechanism of endometriosis is still unclear. Autoimmune thyroid disorders are associated with endometriosis, but the mechanism by which the two diseases are linked is unknown.
Each cell in the body carries protein markers called antigens that allow a cell to be identified as “self” or “non-self” by the immune system. In autoimmune thyroid disorders, the body’s own immune system attacks and damages the thyroid gland. These diseases are characterized by the production of autoantibodies against thyroid-specific antigens, including the thyroid itself and the thyroid-stimulating hormone receptor.
Now, researchers at the Université Paris Descartes looked at the relationship between endometriosis and autoimmune thyroid disorders, specifically at how thyroid disorders affect the progression of endometriosis.
They first found that both the levels of RNA and proteins involved in thyroid metabolism were altered in the biopsied endometrium of patients with endometriosis compared to healthy people. RNA molecules act as templates to make proteins, which perform key functions in the cell.
Moreover, in endometriotic cells, the amount of thyroid hormones was altered compared to that of control cells. The thyroid hormone T4 (thyroxine) is converted into T3 (triiodothyronine), which is much more active than T4. In the endometriotic cells, T4 production was increased while that of T3 was reduced.
The thyroid-stimulating hormone regulates the production of T3 and T4. In vitro (lab) studies using cells from the endometrium of endometriotic patients and healthy controls showed that thyroid-stimulating hormone increased cells’ proliferation. But the researchers saw no differences in the increase of proliferation rate between endometriotic cells and control cells.
Incubating the cells with either the T3 or T4 hormones specifically increased the proliferation and synthesis of the potential harmful reactive oxygen species in ectopic endometrial cells, i.e., cells found outside the normal location of the uterine cavity.
Researchers then used mice to study the effect of thyroid function on endometriosis. In a mouse model with low levels of thyroid hormones, they saw that endometriotic implants were 1.9 times smaller and 1.8 times lighter than in control mice. On the contrary, the endometriotic implants were significantly larger — 58.2 versus 29.8 mm3 — and heavier — 52.3 versus 29.7 milligrams — in a mouse model with increased thyroid hormone levels compared to control mice.
The analysis revealed a positive linear relationship between the concentration of T3 and T4 thyroid hormones and endometriotic implant size, meaning that increasing levels of thyroid hormones may increase endometriotic implant growth.
In a third mouse model, the researchers showed that thyroid autoimmunity did not affect the size of endometriotic implants.
In a retrospective analysis of endometriosis patients with thyroid dysfunction, the results showed no increased prevalence of endometriosis among patients with thyroid dysfunction. The data, however, revealed that in these patients, the existence of thyroid dysfunction was linked with increased chronic pelvic pain and disease severity scores.
Overall, these results suggest that “in humans, thyroid disorders are associated with more severe forms of endometriosis,” researchers stated. “Thyroid function and thyroid hormone medication should be taken into account for the care of women with endometriosis.”